Why HIPAA IT Requirements Matter for Your Healthcare Organization
HIPAA IT requirements are the specific technical, physical, and administrative safeguards mandated by the HIPAA Security Rule to protect electronic protected health information (ePHI). If you handle patient data electronically, you must implement these safeguards to ensure confidentiality, integrity, and availability of that information.
Quick Answer: The Core HIPAA IT Requirements
- Administrative Safeguards – Risk analysis, workforce training, security policies, and incident response procedures
- Physical Safeguards – Facility access controls, workstation security, and secure device/media disposal
- Technical Safeguards – Access controls, audit logs, encryption, and user authentication
- Documentation – Written policies, procedures, and records retained for 6 years
- Business Associate Agreements – Contracts ensuring third-party vendors protect ePHI
The stakes are real. HIPAA violations can result in civil penalties ranging from $137 to $68,928 per violation, with annual maximums reaching nearly $2 million. Criminal violations involving malicious intent can lead to fines up to $250,000 and 10 years imprisonment.
But here’s the good news: HIPAA was designed with flexibility in mind. The regulations recognize that a small medical practice has different needs than a large hospital system. You’re required to implement safeguards that are “reasonable and appropriate” for your organization’s size, complexity, and resources.
For small to medium-sized healthcare providers, the challenge isn’t just understanding what HIPAA requires—it’s figuring out how to implement these requirements without breaking the bank or dedicating your entire team to compliance work.
This guide breaks down the essential HIPAA IT requirements in plain language, helping you understand what you must do, why it matters, and how to approach compliance in a practical, cost-effective way.
Understanding the HIPAA Security Rule’s Core Mandates
The primary purpose of the HIPAA Security Rule is to establish national standards for protecting individuals’ electronic personal health information (ePHI) that is created, received, used, or maintained by a covered entity. It’s about keeping sensitive patient data safe in our increasingly digital world. This rule requires appropriate administrative, physical, and technical safeguards to ensure the confidentiality, integrity, and security of ePHI.
The Security Rule specifically focuses on the safeguarding of ePHI, ensuring its confidentiality, integrity, and availability. This means protecting it from unauthorized access, ensuring it hasn’t been tampered with or destroyed, and making sure authorized users can access it when needed. All HIPAA covered entities and their business associates must comply with this rule, protecting ePHI against reasonably anticipated threats, hazards, and impermissible uses or disclosures. This is a critical component of overall Compliance for Healthcare.
Who is a Covered Entity vs. a Business Associate?
Understanding who is responsible for complying with the HIPAA Security Rule begins with knowing if your organization is a “covered entity” or a “business associate.” These definitions dictate the scope of your HIPAA IT requirements.
A Covered Entity is essentially a healthcare provider, health plan, or healthcare clearinghouse.
- Health Plans: This includes health insurance companies, HMOs, Medicare, Medicaid, and employer-sponsored health plans. There are some exceptions for “excluded benefits” like workers’ compensation, as detailed in §300gg-91 of the Public Health Act.
- Healthcare Providers: Any provider of medical or health services who transmits health information in electronic form in connection with transactions for which HHS has adopted standards. This includes doctors, clinics, hospitals, psychologists, chiropractors, nursing homes, pharmacies, and dentists.
- Healthcare Clearinghouses: Entities that process non-standard health information into a standard format or vice versa.
A Business Associate is a person or entity that performs functions or activities on behalf of a covered entity (or another business associate) that involves the use or disclosure of protected health information. Think of them as the supporting cast in the healthcare data drama. This can include:
- IT providers, like us at Alliance InfoSystems, who manage or service systems containing ePHI.
- Billing companies
- Cloud storage providers
- Claims processing companies
- Data analytics firms
- Transcription services
- Law firms or consultants who handle ePHI
If you’re unsure whether your organization falls into one of these categories, the CMS decision tool can help you determine your status. It’s crucial to get this right, as it forms the foundation of your compliance obligations.
What is Electronic Protected Health Information (ePHI)?
The HIPAA Security Rule’s focus is laser-sharp on electronic protected health information (ePHI). But what exactly is that?
ePHI is essentially any “individually identifiable health information” that is created, received, maintained, or transmitted in electronic media. This means any health information that can be used to identify an individual and is stored or moved electronically. This includes:
- Medical records stored in an Electronic Health Record (EHR) system.
- Emails containing patient information.
- Lab results, prescriptions, and images (like X-rays) stored digitally.
- Billing information sent via secure portals.
- Records of hospital visits and vaccinations.
The key here is “electronic.” While the broader HIPAA Privacy Rule protects all individually identifiable health information in any form (electronic, paper, or oral), the Security Rule specifically addresses the digital field. Safeguarding ePHI is paramount to maintaining Data Integrity Verification and overall patient trust.
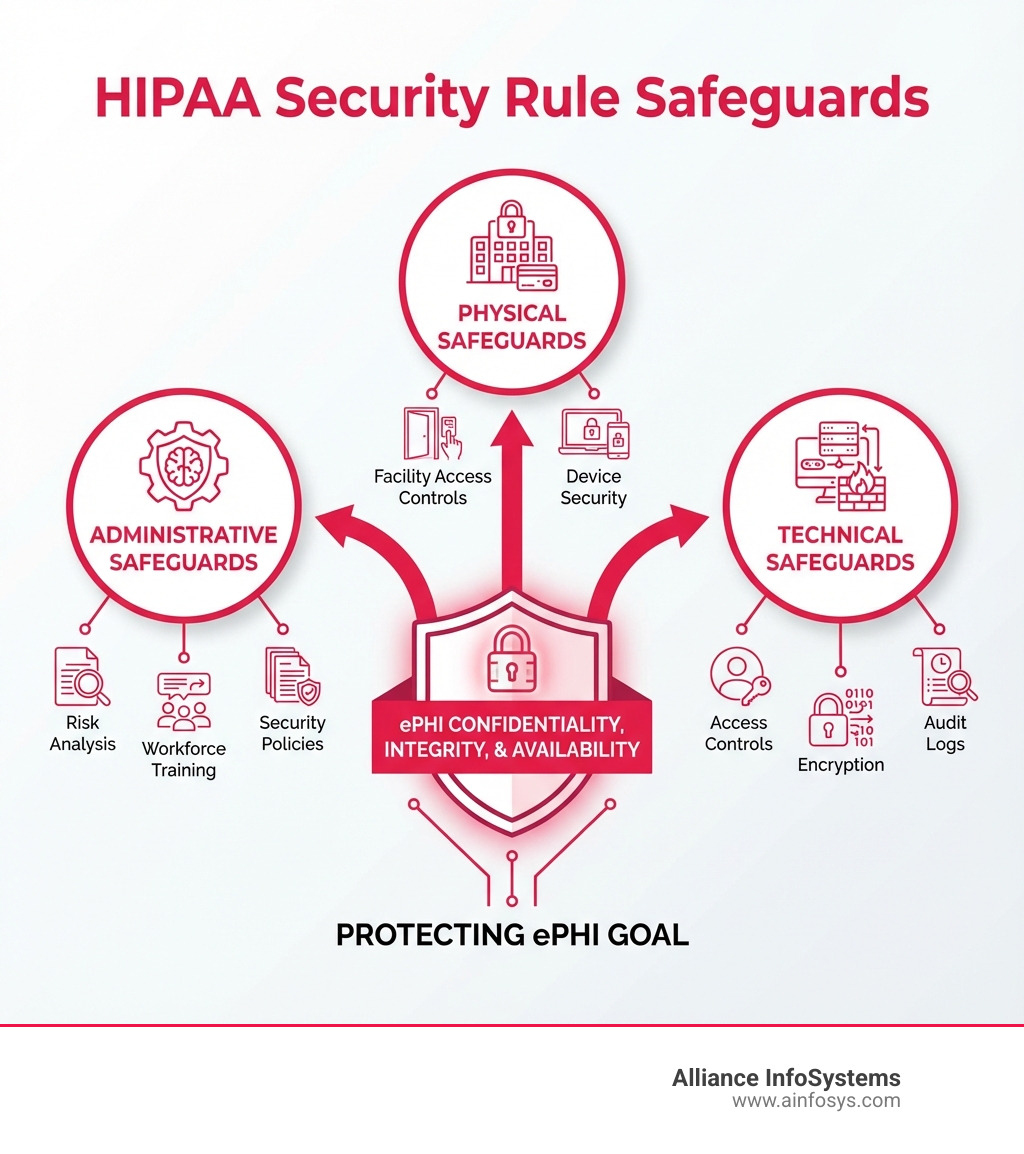
The Three Pillars of HIPAA Security Safeguards
To protect ePHI effectively, the HIPAA Security Rule mandates the implementation of three main categories of safeguards: Administrative, Physical, and Technical. Think of these as the sturdy legs of a stool, all equally important for stability and security.
Administrative Safeguards: The Human Element
Administrative safeguards are the “action-oriented” policies and procedures that manage security measures. They essentially define how an organization will run its security program. These are the human element of security, ensuring that people, not just technology, are part of the solution.
Key administrative safeguards include:
- Security Management Process: We must implement policies and procedures to prevent, detect, contain, and correct security violations. This involves:
- Risk Analysis: Conducting an accurate and thorough assessment of potential risks and vulnerabilities to the confidentiality, integrity, and availability of ePHI. This is the bedrock of your security strategy.
- Risk Management: Implementing security measures that reduce risks and vulnerabilities to a reasonable and appropriate level. This isn’t about eliminating all risk (that’s impossible!), but managing it wisely.
- Sanction Policy: We need to apply appropriate sanctions against workforce members who violate our security policies and procedures. Everyone needs to understand the consequences of non-compliance.
- Information System Activity Review: Regularly reviewing records of information system activity, such as audit logs, to detect potential security breaches.
- Assigned Security Responsibility: Designating a security official who is responsible for developing and implementing our security policies and procedures.
- Workforce Security: Implementing policies and procedures to ensure that all workforce members have appropriate authorization and supervision, and that their access to ePHI is managed from hiring to termination. This includes procedures for granting, modifying, and terminating access.
- Security Awareness Training: Training all workforce members on our security policies and procedures. This isn’t a one-time event; ongoing training is key to maintaining a strong security posture.
- Security Incident Procedures: Implementing policies and procedures to address security incidents, including identifying, responding to, mitigating, and documenting them.
- Contingency Plan: Establishing and implementing procedures for responding to emergencies or other occurrences that damage information systems containing ePHI, including data backup, disaster recovery, and emergency mode operation plans.
- Evaluation: Performing periodic technical and non-technical evaluations of our security policies and procedures to ensure ongoing compliance.
These administrative requirements are crucial for managing Risk effectively and building a culture of security within your organization.
Physical Safeguards: Protecting Your Hardware and Facilities
Physical safeguards cover the physical access to ePHI and the facilities where it’s stored. They’re about keeping unauthorized hands off your sensitive data.
Our physical safeguard requirements include:
- Facility Access Controls: Implementing policies and procedures to limit physical access to our electronic information systems and the facilities that house them, while ensuring that properly authorized access is allowed. This includes mechanisms for controlling access, validating visitors, and documenting repairs and modifications to physical security components.
- Workstation Use: Implementing policies and procedures that specify proper workstation functions, how they’re used, and their physical security. For example, ensuring workstations accessing ePHI are not easily viewable by unauthorized individuals.
- Workstation Security: Implementing physical safeguards for workstations that access ePHI to restrict access only to authorized users. This might involve locking screens or secure boot processes.
- Device and Media Controls: Implementing policies and procedures that govern the receipt, removal, movement, and disposal of hardware and electronic media containing ePHI. This includes:
- Disposal: Implementing policies and procedures for the final disposition of ePHI and the hardware or electronic media on which it is stored.
- Media Re-use: Implementing procedures for removing ePHI from electronic media before the media are re-used.
- Accountability: Maintaining a record of the movements and responsible personnel for hardware and electronic media.
- Data Backup and Recovery: Creating a retrievable exact copy of ePHI when needed. This is where our Data Backup and Recovery services shine, ensuring your data is safe and recoverable.
Key Technical Safeguards for HIPAA IT Requirements
Technical safeguards are the technology and security controls that protect ePHI and control access to it. These are the digital locks and alarms for your data.
Our key technical HIPAA IT requirements include:
- Access Control: Implementing technical policies and procedures for electronic information systems that maintain ePHI to allow access only to those persons or software programs that have been granted access rights. This typically involves:
- Unique User Identification: Assigning a unique name or number for identifying and tracking user identity.
- Emergency Access Procedure: Establishing procedures for obtaining necessary ePHI during an emergency.
- Automatic Logoff: Implementing electronic procedures that terminate an electronic session after a predetermined time of inactivity.
- Encryption/Decryption: Implementing mechanisms to encrypt and decrypt ePHI.
- Audit Controls: Implementing hardware, software, and/or procedural mechanisms to record and examine activity in information systems that contain or use ePHI. These audit trails are vital for forensic analysis and compliance verification.
- Integrity Controls: Implementing policies and procedures to protect ePHI from improper alteration or destruction. This includes electronic mechanisms to corroborate that ePHI has not been altered or destroyed in an unauthorized manner.
- Person or Entity Authentication: Implementing procedures to verify that a person or entity seeking access to ePHI is indeed who or what they claim to be. This can involve passwords, biometrics, or multi-factor authentication.
- Transmission Security: Implementing technical security measures to guard against unauthorized access to ePHI that is being transmitted over an electronic network. This includes:
- Integrity Controls: Ensuring that electronically transmitted ePHI is not improperly modified without detection until disposed of.
- Encryption: Using encryption when transmitting ePHI, especially over open networks like the internet, to prevent unauthorized access.
These technical safeguards are a cornerstone of our Managed Security offerings, designed to keep your ePHI secure.
Implementing and Managing Your HIPAA IT Requirements
The HIPAA Security Rule, located at 45 CFR Part 160 and Subparts A and C of Part 164, is famously flexible, scalable, and technology-neutral. This means it doesn’t prescribe specific technologies or solutions, recognizing that organizations vary greatly in size, complexity, and resources. What works for a small Maryland clinic might not work for a large hospital system, and vice versa. We appreciate this “flexibility of approach” because it allows us to tailor solutions specifically for our clients.
This flexibility, however, doesn’t excuse non-compliance. It simply means we must implement measures that are “reasonable and appropriate” for our specific circumstances. The key is to conduct thorough assessments and document our decisions. This approach also extends to our broader Cybersecurity strategies.
Conducting a Security Risk Analysis
A robust security risk analysis is not just a good idea; it’s a required administrative safeguard under the HIPAA Security Rule. It’s the first and most crucial step in identifying and addressing your HIPAA IT requirements.
The Security Rule requires regulated entities to perform an accurate and thorough assessment of the potential risks and vulnerabilities to the confidentiality, integrity, and availability of ePHI. Here’s how we typically approach it:
- Identify ePHI: We start by mapping where all your ePHI is created, received, maintained, and transmitted within your organization, including systems, applications, and storage locations.
- Identify Threats and Vulnerabilities: We then identify potential threats (e.g., malware, natural disasters, unauthorized access, insider threats) and vulnerabilities (e.g., unpatched software, weak passwords, lack of encryption) that could impact your ePHI.
- Assess Existing Security Measures: We evaluate the security measures you currently have in place to protect against these threats and vulnerabilities.
- Determine Risk Level: For each identified risk, we assess the likelihood of it occurring and the potential impact it would have on your ePHI. This helps us prioritize risks.
- Documentation: All findings, decisions, and mitigation strategies are thoroughly documented.
The HHS Office for Civil Rights (OCR) and the Office of the National Coordinator for Health Information Technology (ONC) have jointly launched a HIPAA Security Risk Assessment Tool that can be incredibly helpful, especially for small and medium-sized healthcare practices and business associates. It’s a valuable resource we often recommend.
Developing Policies and Procedures for HIPAA IT Requirements
Once risks are identified, the next step is to develop and implement policies and procedures that address your HIPAA IT requirements. This is where the distinction between “required” and “addressable” implementation specifications comes into play.
| Implementation Specification | Description |
Required and Addressable are two types of implementation specifications in the Security Rule.
- Required: These specifications must be implemented. No ifs, ands, or buts!
- Addressable: These specifications offer more flexibility. We must assess if they are “reasonable and appropriate” for our organization. If they are, we implement them. If not, we must document why they aren’t reasonable and appropriate, and then implement an equivalent alternative measure if one exists and is reasonable and appropriate. If no reasonable and appropriate alternative exists, we document that as well.
The requirement to adopt reasonable and appropriate policies and procedures is key. These policies and procedures, along with all actions, activities, or assessments required by the Security Rule, must be documented and maintained for at least six years after their creation or the date they were last in effect, whichever is later. This ensures accountability and provides an audit trail. NIST Special Publication 800-66, Revision 2, “Implementing the Health Insurance Portability and Accountability Act (HIPAA) Security Rule: A Cybersecurity Resource Guide,” is an excellent resource for understanding these nuances.
The Impact of HITECH and the Omnibus Rule
The Health Information Technology for Economic and Clinical Health (HITECH) Act, signed into law in 2009 as part of the American Recovery and Reinvestment Act, significantly strengthened HIPAA. Before HITECH, only about 10% of hospitals used Electronic Health Records (EHRs); by 2017, this figure jumped to 86%, largely due to HITECH’s incentives.
HITECH had several profound impacts on HIPAA IT requirements:
- Increased Penalties: It raised the stakes for non-compliance, introducing higher civil money penalties.
- Business Associate Liability: Crucially, HITECH extended direct liability for compliance with the Security Rule (and parts of the Privacy Rule) to business associates. This means business associates can now be held directly accountable for violations, not just through their contracts with covered entities.
- Breach Notification Rule: HITECH introduced the Breach Notification Rule, which mandates that covered entities and business associates notify affected individuals, the Secretary of HHS, and in some cases, the media, following a breach of unsecured protected health information.
- Expanded Patient Rights: It also expanded certain patient rights concerning their health information.
The 2013 Omnibus Final Rule finalized changes to the HIPAA Privacy, Security, Enforcement, and Breach Notification Rules, implementing many of HITECH’s provisions. This rule further cemented the compliance obligations for both covered entities and business associates. Understanding these modifications is essential for navigating today’s HIPAA landscape, as detailed by The Health Information Technology for Economic and Clinical Health Act.
Penalties, Breach Notifications, and Business Associates
Ignoring HIPAA IT requirements can lead to severe consequences. The penalties for non-compliance are tiered based on culpability, ranging from unknowing violations to willful neglect, and can be substantial.
Civil money penalties can range from $137 to $68,928 per violation, with an annual maximum of $2,067,813 for violations of an identical provision. For criminal penalties, a person who knowingly obtains or discloses individually identifiable health information in violation of the Privacy Rule may face a criminal penalty of up to $50,000 and up to one-year imprisonment. If the offense is committed under false pretenses, penalties can increase to $100,000 and up to five years. If there’s an intent to sell, transfer, or use the information for commercial advantage, personal gain, or malicious harm, the penalties can go up to $250,000 and 10 years imprisonment. These penalties are a stark reminder of the importance of preventing Data Loss.
Business Associate Obligations and Agreements (BAAs)
The HITECH Act made business associates directly liable for many of the HIPAA Security Rule’s provisions. This means if you’re a business associate, you’re not just contractually obligated to protect ePHI; you’re legally mandated to do so.
A critical component of this relationship is the Business Associate Agreement (BAA). This is a written contract or other arrangement that must be in place between a covered entity and a business associate, and between a business associate and its subcontractors, if they handle ePHI. The BAA documents satisfactory assurances that the business associate will appropriately safeguard ePHI.
Key components of a BAA include:
- Permitted Uses and Disclosures: Specifying how the business associate is permitted or required to use and disclose ePHI.
- Safeguarding ePHI: Requiring the business associate to implement administrative, physical, and technical safeguards that comply with the Security Rule.
- Reporting Security Incidents: Obligating the business associate to report any security incidents, including breaches of unsecured ePHI, to the covered entity.
- Subcontractor Compliance: Requiring the business associate to ensure that any subcontractors who create, receive, maintain, or transmit ePHI on their behalf agree to the same restrictions and conditions.
- Direct Liability: Acknowledging the business associate’s direct liability for compliance with the Security Rule.
Responding to a Data Breach
Even with the best safeguards in place, breaches can happen. That’s where the Breach Notification Rule comes in. This rule specifies what happens when a security breach involving unsecured PHI occurs. It’s almost impossible to protect data with 100% effectiveness, so organizations need plans to respond quickly and appropriately.
If a breach of unsecured protected health information occurs, covered entities and business associates have specific obligations:
- Notifying Individuals: Affected individuals must be notified without unreasonable delay and in no case later than 60 calendar days after findy of the breach.
- Notifying HHS: The Secretary of HHS must also be notified. For breaches affecting fewer than 500 individuals, organizations have until the end of each calendar year to notify HHS. For breaches affecting 500 or more individuals, HHS must be notified within 60 days.
- Media Notification: If a breach affects 500 or more residents of a state or jurisdiction, prominent media outlets serving that state or jurisdiction must also be notified.
The goal is to Minimize Data Loss and its impact. This rule ensures transparency and allows affected individuals to take steps to protect themselves.
Conclusion: Partnering for Robust HIPAA IT Compliance
Navigating the complex world of HIPAA IT requirements can feel like a daunting task. However, by understanding the core mandates of the Security Rule—the administrative, physical, and technical safeguards—and committing to ongoing management, your organization can build a robust compliance program.
We’ve seen that HIPAA provides flexibility, allowing you to implement safeguards that are “reasonable and appropriate” for your unique environment. But this flexibility comes with responsibility: the need for thorough risk analysis, clear policies and procedures, meticulous documentation, and vigilant monitoring. The HITECH Act and Omnibus Rule have only reinforced these obligations, making business associates directly accountable and increasing the penalties for non-compliance.
At Alliance InfoSystems, we understand the challenges Maryland-based healthcare providers face. Since 2004, our team has been helping organizations like yours implement customized and cost-efficient IT management and security solutions. We believe in a proactive security posture, continuously adapting to new threats and regulatory changes.
For expert guidance on implementing and managing your HIPAA IT security, explore our Managed Security services. We’re here to help you turn the HIPAA maze into a clear, navigable path, ensuring your patient data remains secure and your organization stays compliant. With our IT Support and expertise, you can focus on what you do best: providing excellent healthcare.